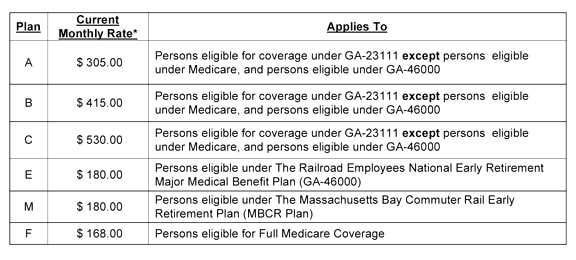
During November and December, UnitedHealthcare will hold an open enrollment under railroad plans GA-23111.
During this open enrollment period, any individual eligible for coverage under one of the GA-23111 plans may enroll and be accepted for coverage without medical underwriting or requirement of good health.
There are no limitations for pre-existing conditions.
Enrollment in November and December is for coverage effective Jan. 1, 2011.
Only those applicants who mail their completed enrollment forms in November or December will be considered for open enrollment.
The next opportunity to enroll during an open enrollment period will not be until November 2012, consistent with the plan’s two-year open enrollment cycle.
This open enrollment is:
- For those covered under any railroad health plan and represented by a railroad labor union.
- For those who are members in accordance with the constitution or bylaws of one of the participating railroad labor unions when coverage under the employer group health plan applying to them ends.
If you, or someone you know, meets the GA-23111 eligibility provisions, open enrollment provides an opportunity to become covered.
You may also enroll your spouse or eligible children if they are not currently covered. In addition, enrollment under Plan F is available for your parent or parent-in-law. Anyone interested in enrolling should call one of the following phone numbers to obtain an enrollment form or additional information:
- For persons eligible for Medicare, call (800) 809-0453.
- For persons NOT eligible for Medicare, call (800) 842-5252.
Note: Enrollment during November and December of the open enrollment period provides for coverage effective the following calendar year, Jan. 1 through Dec. 31. Each June 1 of that calendar year, and only at that time, adjustments to the premium for all plans under GA-23111 may occur. Additionally, if you are enrolled in either Plan A, B or C under GA-23111, and a change in the premium amount you pay does occur, you will be allowed, at that time, to switch your plan to a different plan (A, B, or C) with a lower premium, if available.
Related News
- Razor blade found on brake wheel
- Coming Soon: SMART-TD Voluntary Income & Life Protection (VILP) Program
- Senate Passes Tax Bill Without Including Railroaders
- SMART-TD Honors the Retirement of Brother Greg Hynes: A Visionary, a Fighter, and a Legend
- SMART-TD Calls on U.S. Senate to Support the Cantwell Amendment and Protect Rail Workers
- Yardmaster Protection Act Introduced
- PHOTO GALLERY: 2025 Denver Regional Training Seminar
- Fighting for Stronger Heat Protections for Rail Workers
- Regional Training Seminar Sets (Mile-High) Record in Denver
- Registration Open for Anaheim Regional Training Seminar